Diabetes and Oral Health: Specialized Preventive Advice for Joplin’s Diabetic Community
Living with diabetes means paying closer attention to many parts of your health, and oral care is often overlooked. Diabetes can weaken the body’s immune response, making it harder to fight infections anywhere including the mouth. When blood sugar levels fluctuate, the balance of bacteria in the oral environment can shift, increasing the risk of inflammation and slow healing.
In Joplin, daily life often revolves around shared meals, church gatherings, school events, and community activities. Oral discomfort or untreated gum issues can quietly interfere with those moments long before pain becomes obvious. The connection between blood sugar control and oral health is strong, but it does not have to be complicated or overwhelming.
This guide is designed to offer practical, preventive insight, clear explanations without medical jargon. You will learn how diabetes affects the mouth, what early signs to watch for, and how consistent care supports long-term comfort and overall wellness.
How Diabetes Affects Oral Health
Diabetes changes how the body manages inflammation and infection, and the mouth is especially sensitive to these shifts. One of the most common effects is reduced saliva flow. Saliva plays a protective role by washing away food particles and neutralizing acids. When saliva production drops, the mouth becomes drier and more vulnerable to bacterial buildup.
Higher blood sugar levels also create an environment where harmful bacteria thrive. This can increase plaque formation along the gumline, even when daily habits remain the same. Over time, these bacteria trigger inflammation in the gums and surrounding tissues.
Healing is another concern. Diabetes can slow blood circulation, which means gum tissue may take longer to recover from irritation, dental procedures, or minor injuries. Inflammation may linger longer than expected, increasing discomfort and the risk of progression.
Together, dry mouth, bacterial imbalance, slower healing, and heightened inflammation explain why oral health risks increase with diabetes. Understanding these changes helps patients take proactive steps rather than reacting only when symptoms appear.
Common Oral Health Issues Seen in Diabetic Patients
Oral health changes linked to diabetes often develop gradually and may not cause pain at first. This makes awareness especially important.
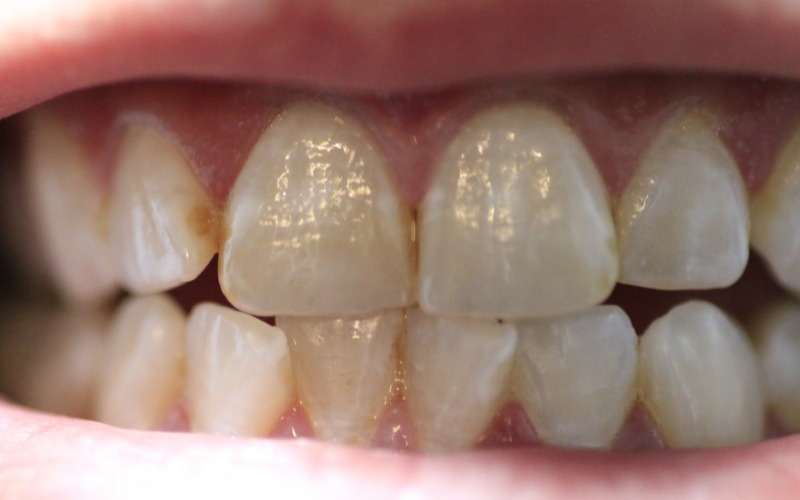
- Gum inflammation and periodontal disease: Gums may appear red, swollen, or tender, sometimes without noticeable discomfort.
- Frequent infections or sores: Small irritations can become recurring problems due to reduced immune response.
- Tooth sensitivity and decay: Dry mouth and bacterial growth increase exposure to acids that weaken enamel.
- Changes in taste or burning sensations: Nerve sensitivity and oral dryness can alter how food tastes or feels.
- Delayed healing after dental procedures: Recovery may take longer, even after routine treatments.
Because these issues often progress quietly, many people do not seek care until damage is more advanced. Regular monitoring helps catch subtle changes early, supporting comfort and stability before problems interfere with daily life.
The Two-Way Relationship Between Blood Sugar and Gum Health
Diabetes and gum health influence each other in both directions. When blood sugar levels remain elevated, the body’s inflammatory response intensifies. This makes gum tissue more vulnerable to infection and breakdown, increasing the likelihood of periodontal disease.
At the same time, chronic gum inflammation does not stay confined to the mouth. Inflammatory signals can enter the bloodstream, making it harder for the body to regulate glucose levels. This means untreated gum disease may contribute to more unstable blood sugar control.
This cycle explains why oral care is considered part of overall diabetes management. Preventive steps, such as a routine preventive checkup in Joplin, help reduce inflammation before it becomes systemic. By controlling oral infection, patients often support better balance throughout the body.
Breaking this cycle does not require extreme measures. Consistent monitoring, early intervention, and professional guidance help stabilize both oral health and blood sugar over time.
Specialized Preventive Dental Care for People With Diabetes
More Frequent Preventive Exams
For patients with diabetes, routine dental visits serve as an early warning system. Subtle gum changes, dryness, or inflammation can be identified before symptoms become disruptive. These visits allow providers to tailor care based on how diabetes is affecting oral tissues at that time.
Professional Cleanings to Reduce Inflammation
Professional cleanings remove plaque and bacteria that daily routines may miss, especially near the gumline. Reducing this bacterial load lowers the risk of infection and helps calm inflammation that can impact blood sugar regulation.
Monitoring Gum Health Changes Over Time
Tracking gum measurements, tissue response, and healing patterns over multiple visits helps identify trends early. This ongoing assessment allows adjustments before minor concerns turn into chronic issues.
At Joplin Family Dental, preventive care for diabetic patients focuses on consistency and clear communication. A structured preventive checkup plan helps patients stay ahead of changes while supporting comfort, stability, and long-term oral wellness.
Daily Oral Care Tips Tailored for Diabetic Patients
Daily habits play a key role in supporting professional care. For people with diabetes, small adjustments make a meaningful difference.
- Managing dry mouth: Stay hydrated and be mindful of medications that may reduce saliva flow.
- Timing oral care around meals and medications: Cleaning the mouth after meals helps reduce sugar exposure and bacterial growth.
- Recognizing early warning signs: Persistent dryness, tenderness, or bleeding deserve attention even without pain.
Consistency matters more than intensity. Daily awareness supports early action and helps prevent escalation between visits.
When Diabetic Patients Should See a Dentist Sooner
Some symptoms should never be ignored, especially for individuals managing diabetes.
- Bleeding gums
- Persistent bad breath
- Loose teeth
- Mouth sores that do not heal
- Pain or swelling
These signs may indicate infection or inflammation that requires timely evaluation. Seeking care early supports healing and reduces complications, reinforcing trust and long-term oral stability.
Why Preventive Dental Care Matters for Joplin’s Diabetic Community
Joplin is an active community where people value staying engaged, whether attending school events, volunteering, or enjoying local restaurants. Oral discomfort can quietly limit those experiences. Preventive dental care supports comfort, confidence, and overall wellness.
With access to strong local healthcare resources, consistency becomes a lifestyle habit rather than a reaction to problems. Preventive routines help diabetic patients protect not only their smiles, but also their ability to stay active and connected.
Diabetes and oral health are closely connected. Inflammation, healing, and blood sugar balance all influence what happens in the mouth. Preventive care helps interrupt that cycle before discomfort or complications arise.
Staying proactive supports long-term stability and peace of mind. If you are managing diabetes and want to protect your oral health, scheduling a preventive visit is a practical next step. The team at Joplin Family Dental is here to support consistent, informed care that fits your daily life and long-term health goals.
What People Want to Know About Preventive Checkups?
Persistent bad breath may result from dry mouth, bacterial buildup, or gum disease. These issues are more common when diabetes affects saliva flow and immune response.
Yes. Inflammation in the mouth can contribute to systemic inflammation, which may interfere with diabetes management and increase health risks over time.
They may be. Dry mouth and higher sugar levels in saliva increase acid production, which can weaken enamel and raise cavity risk.
Sometimes. Symptoms may be subtle at first, and healing delays can mask severity. Regular evaluations help identify problems early.
Yes. Smoking further reduces blood flow and healing ability, significantly increasing the risk of gum disease and tooth loss in diabetic patients.